What is uveitis?
Uveitis is an inflammation of the middle of the three layers of tissue in the eye, known as uvea.
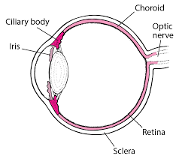
The uvea is made up of a number of different parts, including the iris at the front, the choroid at the back, and the ciliary body in between. Iritis, inflammation of the iris, is the most common form of uveitis and may also be called anterior uveitis.
What are the symptoms?
Symptoms of uveitis include:
- Redness
- Eye pain
- Sensitivity to light
- Weepy or teary eyes (watering)
- Black dots in the vision (floaters)
- Blurry vision
- A pupil that is smaller than normal.
Symptoms may occur in just one eye or in both eyes at the same time.
What causes uveitis?
Uveitis can be caused by eye infections or by isolated problems, such as scratch to the cornea. However, in people with axial spondyloarthritis (axSpA), uveitis is most often caused by the same process that causes inflammation of the joints.
It is thought smoking also increases the chances of uveitis, including in those with underlying inflammatory causes, such as axSpA.
How is it diagnosed?
Your doctor will diagnose uveitis by talking to you about your symptoms and asking about any other medical conditions you have, like axSpA. If you are already seeing an optometrist, they may also be able to pick up changes in your eye and identify them as uveitis. Your doctor will most likely refer you to an ophthalmologist to have the uveitis confirmed by a thorough eye exam. An ophthalmologist is a medical doctor who has done extra training in the diagnosis and management of conditions that affect the eye or the visual system. The ophthalmologist will work with you and the other members of your healthcare team to figure out the best treatment for you.
What will happen to me?
For most people with uveitis, the disease will be manageable with the right treatment and symptoms will ease. There will be times when the inflammation and symptoms are minimal. However, as with axSpA, uveitis symptoms may worsen at times. This is more likely to happen when the other symptoms of axSpA also worsen, or ‘flare’. Some cases of uveitis can cause long-term damage to the eye. While uncommon, permanent loss of vision can occur. However, if uveitis is diagnosed and treated early enough, in most cases these long-term complications can be avoided. This is why it is important to see your doctor should you experience symptoms you suspect might be uveitis.
Can uveitis be cured?
While there may be times when you experience no signs or symptoms of uveitis, unfortunately, it is not curable, except where it is caused by a bacterial infection. Instead, the aim of treatment is to control the symptoms and prevent long-term damage and complications.
What treatments are there for uveitis?
There are two main medications that are used to treat uveitis. Your ophthalmologist will prescribe either of the following, or a combination of the two:
- Corticosteroids to reduce the eye inflammation
- Eye drops or cream that dilate the pupil to prevent it sticking to the lens of the eye and causing scarring.
In addition, if you are not already taking them for your axSpA, anti-inflammatory, immunosuppressant or immunomodulatory medication may be recommended to treat the underlying cause of the uveitis. Your rheumatologist will be able to discuss this with you.
What can I do?
There are a number of things that you can do to reduce the risk of long-term complications from uveitis and ensure you are an active member of your healthcare team.
- Ensure that your axSpA is well-managed as this will keep the inflammatory process that causes uveitis under control as well.
- Monitoring symptoms and taking your medications as prescribed will reduce the risk of long-term damage to your eyes.
- To minimise the long-term side effects of some medicines, you will be prescribed the lowest possible dose to control your symptoms, so taking them as prescribed is particularly important.
- Your ophthalmologist may need to see you regularly while you are taking your medicines to treat your uveitis. Ask how often you need to see them.
- Speak with your doctor if you have any questions about the treatments you have been prescribed or about uveitis itself.
- When discussing possible treatments, you may want to ask your doctor:
- how long it will take for your medication to start working. With some medication it can be several weeks before you start to see an improvement in your condition
- what some of the possible side effects might be, what the signs of these side effects are and what you should do if you think you are experiencing a side effect
- when you can stop taking your medication. Some medication may only need to be taken until the symptoms go away while others may need to be taken for longer.
- When discussing treatment with your doctor, tell them about any medication you are taking, including complementary medications. Some medications can interact causing unwanted side effects. It is best if your doctor knows exactly what you are taking so that they can try and recommend medicines that don’t have these interactions.
- Speak with your GP about seeing a counsellor or psychologist if you feel you need to talk to someone about the impact uveitis or axSpA is having on your mental wellbeing.
This resource has been developed based on the best available evidence. A full list of references is available upon request.









